Ozempic (Semaglutide): Mechanisms, Pharmacology, and Research Considerations
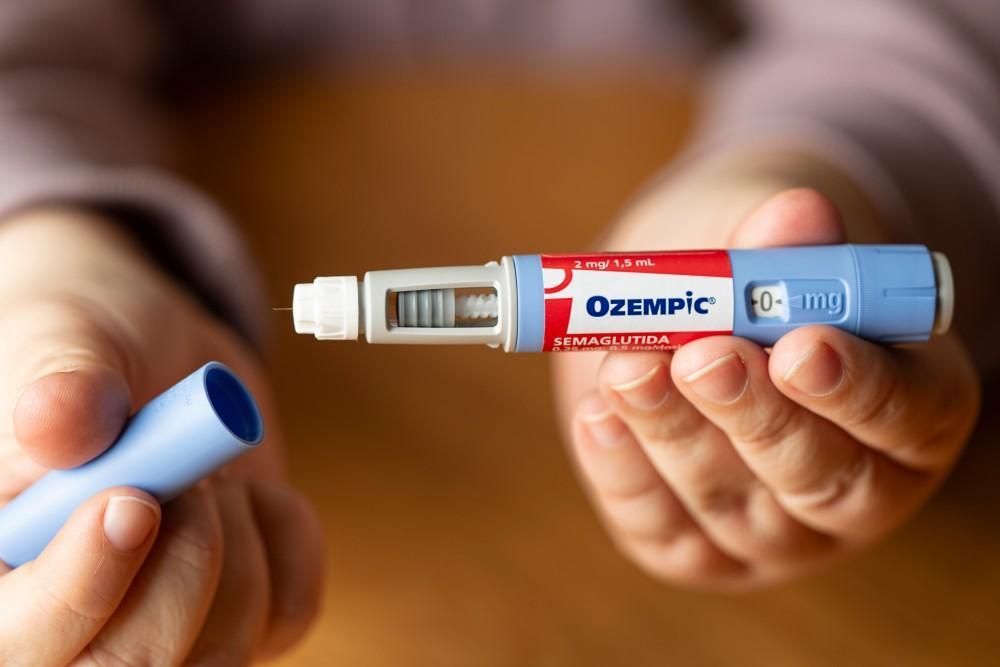
On a Tuesday morning in a university lab, a postdoc set up a GLP‑1 receptor internalization assay using frozen islets from C57BL/6 mice. The protocol called for a long‑acting GLP‑1 analogue as a positive control. Semaglutide was the obvious choice; its once‑weekly clinical profile and albumin‑binding chemistry make it interesting both as a tool compound and as a probe of prolonged receptor engagement. The results that week shifted how the group designed their chronic dosing window.
What is Ozempic (semaglutide)? Ozempic is the trade name for semaglutide, a synthetic peptide agonist of the glucagon‑like peptide‑1 receptor (GLP‑1R). Clinically it has been approved in several formulations for glycaemic management and, in a higher‑dose formulation, for chronic weight management; those approvals are regulatory facts, not experimental recommendations. For bench scientists, semaglutide functions as a long‑acting GLP‑1R agonist with pharmacologic behavior distinct from short‑acting native GLP‑1 or exenatide. Semaglutide is designed to engage GLP‑1R for an extended period after a single subcutaneous exposure. That prolonged activity is a product of two design choices: single‑amino‑acid substitutions that reduce proteolytic cleavage, and a fatty‑acid modification that promotes reversible albumin binding. Together they change tissue exposure and receptor kinetics.
Molecular mechanism and receptor pharmacology GLP‑1R is a class B G protein‑coupled receptor (GPCR) that couples primarily to Gs, elevating intracellular cAMP in target cells. Semaglutide is a full agonist at GLP‑1R in classical cAMP assays, but like many peptide agonists it shows context‑dependent signaling: potency and the balance between G protein versus beta‑arrestin pathways can shift by cell type and assay. Three pharmacologic features matter for experimental design:
High intrinsic potency: semaglutide produces strong cAMP responses at low‑nanomolar to sub‑nanomolar concentrations in heterologous assays. Prolonged receptor engagement: the albumin‑binding motif increases systemic residence time, so receptor occupancy lasts far longer than for unmodified GLP‑1. Receptor internalization and desensitization dynamics: prolonged exposure changes internalization kinetics and downstream signaling profiles compared with acute agonists.
Pharmacokinetics and formulation basics for researchers For preclinical planning it helps to think in terms of three time domains: acute (minutes–hours), subacute (days), and chronic (weeks–months). Semaglutide's clinical half‑life is about one week, which translates into a sustained exposure profile after a single subcutaneous administration. In rodents, pharmacokinetics differ: clearance is faster and absolute exposure depends on species, formulation, and injection site. Formulation matters. Clinically, semaglutide is delivered as a sterile, preservative‑free solution for subcutaneous injection. For laboratory use, suppliers provide lyophilized peptide that requires proper reconstitution and cold‑chain handling. Stability after reconstitution and repeated freeze–thaw cycles varies by vendor; check certificates of analysis and stability data before use in multi‑week studies.
Clinical trial signals that inform mechanistic hypotheses Large randomized trials have generated effect sizes and safety signals that are useful reference points for mechanistic research, provided the interpretation stays within a preclinical frame. Key trials include the SUSTAIN program (glycaemic outcomes) and the STEP program (weight management). STEP 1 reported mean placebo‑subtracted weight loss in the double‑blind cohort on the higher‑dose semaglutide regimen measured over 68 weeks; the absolute numbers helped drive hypotheses about appetite‑ and reward‑circuit modulation. Safety findings in clinical datasets point to mechanistic questions worth studying in animals and cells: gastrointestinal side effects (nausea, vomiting), increased cholelithiasis/cholecystitis signals in some analyses, and a signal for retinopathy complications in SUSTAIN‑6 among patients with pre‑existing diabetic retinopathy. Pancreatitis reports have been inconsistent across post‑marketing surveillance and trials. None of these signals should be read as conclusive causation, but they highlight pathways—gut motility, bile metabolism, retinal microvasculature—worth modeling experimentally.
Nausea and related GI effects: frequently reported across trials (often 20–40% incidence depending on dose and population). Retinopathy signal: an increased incidence of retinopathy complications in SUSTAIN‑6 prompted mechanistic follow‑up research. Cardiovascular outcomes: some semaglutide trials have shown reduced major adverse cardiovascular events versus placebo in high‑risk cohorts, an observation that stimulated work on vascular and anti‑inflammatory mechanisms.
Assays and models for semaglutide research Semaglutide can serve in vitro and in vivo as a probe of sustained GLP‑1R activation. Choose assays that match the temporal and signaling questions you plan to ask.
Acute signaling: cAMP accumulation (HTRF or ELISA), PKA activation, and CREB phosphorylation are standard readouts for minutes–hours after agonist addition. Desensitization/internalization: beta‑arrestin recruitment assays, receptor internalization by confocal imaging, and surface receptor ELISA give insight into receptor trafficking after prolonged exposure. Cell models: HEK293 cells engineered to express human GLP‑1R are common for receptor pharmacology. Pancreatic beta‑cell lines (INS‑1, MIN6) and primary islets add physiology but introduce variability in receptor expression and coupling. In vivo endpoints: glucose tolerance tests, food‑intake monitoring, energy‑expenditure by indirect calorimetry, body‑weight trajectories, and histologic endpoints (islet morphology, gut transit, gallbladder/bile composition) are typical.
Practical tips for in vitro work When planning dose–response curves, include both a short exposure (30–60 minutes) and a prolonged exposure (24–72 hours) to capture signaling bias and receptor regulation differences. For internalization assays, sample multiple time points in the first 2–6 hours and again after 24 hours to see recovery or sustained down‑regulation. If using albumin in culture media, be aware that semaglutide’s albumin binding will affect free fraction and apparent potency.
Analogue chemistry and design features (high level) Semaglutide's design illustrates two common peptide strategies: protease resistance through selective amino‑acid substitution, and half‑life extension through reversible serum protein binding. The second strategy typically uses a lipophilic acyl chain attached via a spacer to a lysine side chain; reversible binding to albumin slows renal clearance and alters distribution. For researchers working on new analogues, the trade‑offs are familiar. Increasing lipophilicity raises residence time but can change tissue partitioning and receptor kinetics. Substitutions that block DPP‑4 cleavage prolong peptide life, but may also alter receptor binding and immunogenic potential. Analytical work—mass spectrometry, peptide mapping, and bioactivity assays—must accompany any modification to confirm retained receptor agonism.
Comparative landscape: other GLP‑1 agents and research alternatives Comparing semaglutide to other GLP‑1R agents clarifies experimental choices. Short‑acting agonists highlight acute signaling; long‑acting molecules probe sustained receptor engagement. Multi‑agonists (e.g., GLP‑1/GIP or GLP‑1/glucagon co‑agonists) introduce additional receptor biology and metabolic readouts. If your lab needs GLP‑1 pathway probes optimized for specific experimental goals, consider available analogues that mimic different aspects of semaglutide's profile: single‑pathway GLP‑1 analogues for focused receptor work, or multi‑pathway constructs when studying integrated metabolic responses.
Safety, regulatory, and procurement considerations for labs All peptides you acquire should be handled as research‑use‑only materials. Do not repurpose for human or veterinary use. Institutional approval and appropriate biosafety oversight are required for animal studies and for any human‑derived biological materials used in assays. Storage and handling basics: unopened lyophilized peptide generally ships on cold packs and is best stored at −20°C or below for long‑term retention of potency, unless the certificate of analysis specifies another condition. After reconstitution, stability varies; many vendors recommend refrigeration and limited time at 2–8°C. Repeated freeze–thaw cycles can accelerate degradation. Run analytical QC—HPLC purity, mass spec verification, and endotoxin testing—before committing material to long multi‑week experiments. Regulatory notes: import/export rules differ by country and by peptide class. Some jurisdictions place restrictions on analogues that are clinically relevant or structurally similar to approved drugs. Check institutional procurement policies and, when relevant, consult export control or legal counsel for compliance.
Practical experimental endpoints and study designs Match endpoints to mechanism. If your interest is receptor pharmacology, focus on in vitro signaling and trafficking. If you want systemic metabolic readouts, design a study with appropriate length to detect changes in food intake or body composition. A few sample study frameworks used in the literature:
Acute pharmacodynamics: single dose, sample blood for hormone and metabolite responses from minutes to 24 hours; use glucose tolerance tests to probe insulinotropic action. Subchronic mechanistic work: repeated dosing over 2–4 weeks to study receptor desensitization, appetite regulation, and early tissue remodeling. Chronic adaptation: multi‑month studies for body composition, liver fat, pancreatic histology, and behavioral endpoints related to reward and palatability.
Outcome measures commonly include:
Physiological: body weight, food intake, energy expenditure, glucose homeostasis readouts. Molecular: receptor expression, downstream kinase activation, transcriptomics in target tissues. Histologic: islet architecture, enteroendocrine cell counts, bile duct and gallbladder pathology.
Closing notes: anchoring the science to the lab bench Back in that university lab, the postdoc adjusted the chronic dosing window after seeing prolonged GLP‑1R internalization with semaglutide in primary islets. The tweak let the team distinguish between transient signaling and longer‑term adaptation in insulin secretion. Semaglutide is a useful tool for probing sustained GLP‑1R engagement, but only if experimental design accounts for its protease resistance and albumin‑bound pharmacokinetics. Handle it as the potent, long‑acting probe it is, and design assays that respect both its acute and chronic behavior.
Research use only: This article is informational and intended for laboratory research planning. Semaglutide and related products discussed here are not to be used in humans outside of approved clinical contexts. Always follow institutional, local, and federal regulations for procurement and use.